The indications for intramedullary nailing of humeral shaft fractures have now been expanded because it is less invasive than plate fixation. However, there are multiple neurovessels in the distal humerus, and the anatomy is relatively complex. Distal locking of an intramedullary nail increases the risk of infection and nerve damage, as well as increased operative and fluoroscopy time.
Since the bone shape of the distal humerus appears to be suitable for initial stability of a long intramedullary nail, is there no need for distal locking to control rotation after nail placement.
Some scholars have hypothesized that if sufficient rotational stability is confirmed intraoperatively, distal locking of long IM nails is unnecessary and the fracture does not involve the distal third. This does not affect healing and functional recovery, but reduces surgical time, fluoroscopy time and risk of nerve damage.
Scholars compared the results of IM nails with and without distal locking on a case-by-case basis.
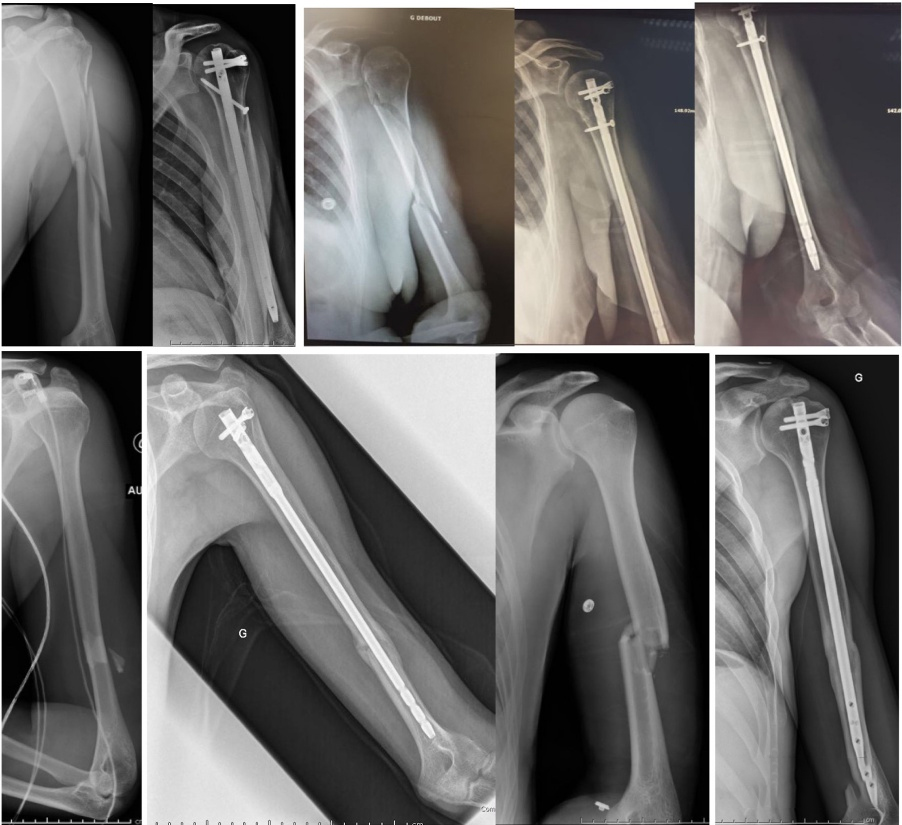
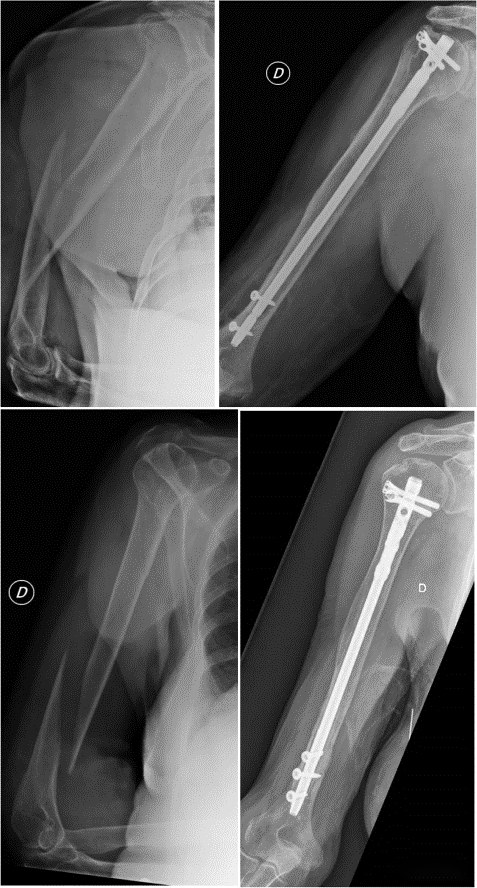
Note: IM nailed an instance of gratuitous locking. The case had a midshaft fracture and was fixed with transverse screws at the proximal short incision via percutaneous internal fixation.
Note: The middle and lower 1/3 of the humeral shaft is fractured, and the distal end is locked and fixed.
Conclusion:
Studies have shown that if intramedullary nailing is stable in the distal fragment, there is no difference in healing rates and function compared to distal locking.
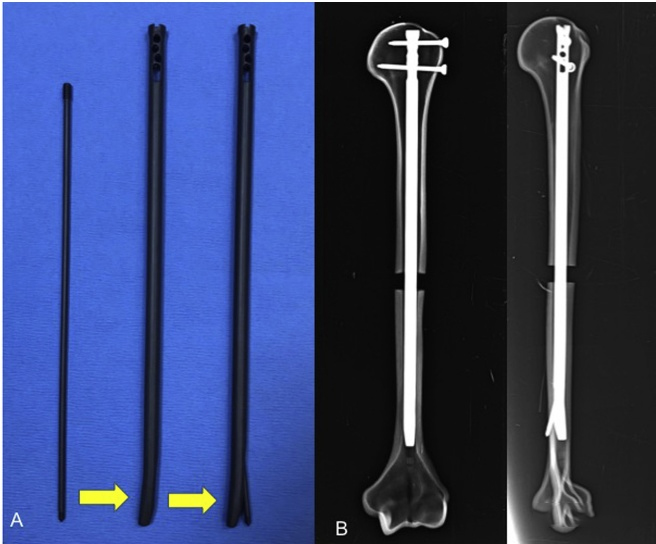
Of course, in our daily work, we are still worried that the distal end of the intramedullary nail will not be locked, resulting in instability. Here is a special intramedullary nail (InSafeLOCK Humeral Nail (TST)) invented by foreign scholars for your reference.
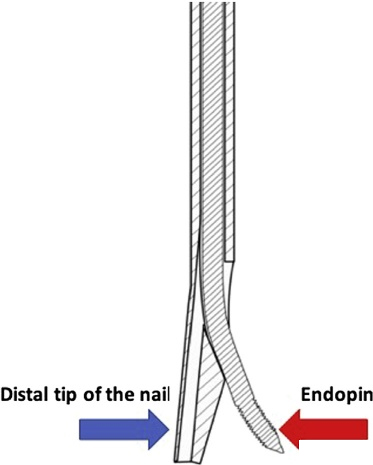
Special structure of the head end of InSafeLOCK Humeral Nail (TST):
After biomechanical testing, both this nail and the ordinary intramedullary nail have sufficient stability after axial and rotational loading.
Precautions for distal locking placement of ordinary intramedullary nails:
- In most cases, vascular forceps should be used to bluntly separate the soft tissue to reach the bone surface before drilling any interlocking screws to minimize neurovascular damage.
- When distal interlocking screws are used: Making a relatively large incision can provide a better field of view and avoid damage to nerves and blood vessels.
- When screwing in the distal interlocking screw, rotate the C-arm machine 180°, and its top can be used as an operating table to support the upper arm to insert the distal interlocking screw.
Disclaimer: This article comes from professional journals and books and is edited by Orthopedic Garden. If you have any copyright issues, please contact us.
Post time: Nov-02-2023

.jpg)